It’s often called the “silent epidemic.”
Worldwide, 540 million adults are living with diabetes but over half are unaware they have the disease.
Diabetes robs people of their quality of life, sometimes taking livelihoods, hope and, if left untreated, even lives.
Diabetes is one of the world’s greatest public health crises. The International Diabetes Federation predicts this global burden will only grow, impacting one in eight adults by 2045.
The disease hits hardest among people in low- and middle-income countries where three in four adults with diabetes live. For those in poverty, it can unravel the delicate equilibrium of their lives, forcing them over the threshold of financial instability.
Having witnessed firsthand the impact of the rising diabetes epidemic on sponsored families, Unbound and its Quezon program in the Philippines began a partnership with a Nebraska-based nonprofit organization called Chronic Care International (CCI).
In 2023, after years of deliberation and research, the organizations launched phase one of a two-phase noncommunicable diseases pilot program. The program seeks to improve health outcomes of elder adults in the Philippines who have diabetes and live in poverty.
The phase-one results so far have exceeded expectations and could one day set the partnering organizations on a path to creating a low-cost global health care model for the practical management of diabetes that could be replicated in other developing countries.
June 13, 2024 | Partnerships
Diabetes pilot program fights the ‘silent epidemic’ with a low-cost care model
Unbound and partner Chronic Care International are helping sponsored elders in the Philippines manage their diabetes
By Kati Burns Mallows

Sponsored elder Geronimo, a former taxi driver turned entrepreneur, improved his quality of life by learning to manage his Type 2 diabetes through Unbound and CCI’s noncommunicable diseases pilot in the Philippines.
The problem with diabetes management in developing countries
Staff with Unbound’s programs have been witnessing the impact of the diabetes epidemic on sponsored individuals and their families for many years. During home visits, staff frequently see the disease chipping away at the fragile headway some families have made in improving their situations because the household’s main provider is too sick to work.
“The success of our sponsorship program really depends on our families being able to take the initiative to build their own paths out of poverty,” said Dan Pearson, Unbound’s chief international program officer. “But that kind of expectation is not intuitive when someone is dealing with a chronic disease.”
Globally, noncommunicable diseases are responsible for 74% of all deaths, according to the World Health Organization. Noncommunicable diseases (also known as chronic diseases) disproportionately affect people who live in poverty — 86% of all deaths from noncommunicable diseases before age 70 occur in low- and middle-income countries.
Across the three regions of the world where Unbound has a presence, diabetes and hypertension (high blood pressure) are on the rise, Pearson said. In addition, in the countries where Unbound works, staff have noted increasing demands on health care systems where the primary focus has been on working with communicable diseases, like malaria or HIV, and improving the survival rates of children under age 5.
As the population of older adults increases worldwide — which is one major driver of the diabetes epidemic — the disease burden in these countries is evolving, shifting from communicable to noncommunicable diseases.
“Our belief is that it will take decades for these health systems to really make the adjustments they need to make in order to serve the changing needs of their populations,” Pearson said.
Pearson knew Unbound staff lacked the medical expertise to support the additional challenges families impacted by diabetes were facing.
Then, almost 10 years ago, a physician with that outside expertise approached Unbound with similar concerns about the epidemic’s impact on marginalized populations and asked for help formulating a solution to the problem.

Nenita, a 79-year-old sponsored elder in the noncommunicable diseases pilot program, sits outside a family member’s home in the Philippines. She spent a week in the hospital for extreme vomiting five years ago when she found out she had diabetes. Thanks to the pilot, she now has access to medications that help her manage the disease.
How the diabetes epidemic brought together two partnering organizations on similar paths to help people in poverty
Dr. Hans Dethlefs, a primary care physician and president and medical director of CCI, has been focused on diabetes management and quality improvement for much of his medical career.
Dethlefs was volunteering his medical expertise to treat sponsored children in Unbound’s Honduras program more than 25 years ago when he first encountered the disease’s impact on people who live in poverty.
When a colleague founded Chronic Care International in 2009, Dethlefs joined the team of volunteer doctors, health care specialists and global health experts united by a common goal: transforming health care in underserved communities in developing countries, with a specific focus on diabetes care.
CCI partners with others to create a unique framework of medical resources, education, patient cooperatives and outcomes measurement that enables sustainable long-term care. For the last decade, Dethlefs worked with CCI’s diabetes and high blood pressure program in the Dominican Republic, a place where those two illnesses have become the culprits for three quarters of all emergency room visits.

At the pilot clinic inside Unbound’s project office in the Philippines, Dr. Hans Dethlefs checks the feet of sponsored elder Aurelia, who is a diabetes patient in the noncommunicable diseases pilot. Dethlefs is assisted by Isabella Bunag, a Filipino physician and member of the new health care team hired for the pilot.
As CCI grew in understanding barriers to care their patients faced, Dethlefs could see that most individuals who live in poverty are unable to pay the incremental cost to see the doctor, get lab tests and buy medications.
“What ends up happening is that they go either untreated or undertreated, and so they develop health complications at a much younger age and have shorter lifespans, which has a cascade effect on the rest of their family,” Dethlefs said.
By purchasing generic medications in bulk and training a local health care team, CCI learned they could provide essential care to individuals with diabetes and high blood pressure for a cost that was similar to that of a monthly sponsorship.
With that knowledge, Dethlefs reached out to Pearson to see if Unbound would be the sponsorship organization behind CCI’s model of care.
Dethlefs believes Unbound is a great partner for CCI’s model of care because the nature of Unbound’s work since the organization’s founding more than 40 years ago has included supporting families in overcoming social determinants of health.
Environmental and social factors can adversely affect a patient’s ability to get proper care, but Unbound staff work to eliminate these types of hindrances, like helping families with access to transportation and nutrition, and having social workers visit families in their homes to monitor progress.
“It’s really an ideal partnership to have a health care-focused organization like CCI and a social determinant of health-focused organization like Unbound coming together,” Dethlefs said.
The organizations launched phase one of a noncommunicable diseases pilot program with Unbound’s Quezon program in the Philippines in February 2023. For phase one, using best practices gleaned from their programs in the Dominican Republic, CCI began testing their model of care on 158 participants from Unbound’s sponsored elders program who were largely living with Type 2 diabetes and high blood pressure.
“Our hope is that we can figure out how to provide a model for low-cost intervention to help people manage their diabetes,” Pearson said. “Then we can not only help the families we’re serving right now in the Philippines, but we can also provide a model of care to other NGOs and potentially the Filipino government.”

Physicians with Chronic Care International, Unbound Quezon staff and members of the new health care team for the pilot program gather to discuss the day’s plans ahead of visiting patients in their homes. The CCI team travels to the Philippines periodically to evaluate the pilot program.

The noncommunicable diseases pilot is a partnership between Unbound, Unbound’s Quezon program and Chronic Care International. Pictured are members of all three teams at the Quezon program office in February 2024, including Dan Pearson (left, back row), Unbound’s chief international programs officer; Malou Navio (left, front row), Unbound regional project director; and members of the CCI team including Dr. Jeremy Howe (middle left, back row), Dr. Hans Dethlefs (middle right, back row), Corey Lawson (right, back row), Kim Howe (middle, front row) and Andrea Dethlefs (right, front row).

Unbound’s program and health care teams work to get basic medications imported in bulk into the Philippines at a lower cost for pilot patients.
Our hope is that we can figure out how to provide a model for low-cost intervention to help people manage their diabetes. Then we can not only help the families we’re serving right now in the Philippines, but we can also provide a model of care to other NGOs and potentially the Filipino government
— Dan Pearson, Unbound chief international program officer
PILOT OUTCOMES: The elder who received care just in time
When Dethlefs thinks about some of the worst-case scenarios for individuals with diabetes and high blood pressure, he mentions heart attacks, vision loss, amputations, kidney failure and even death.
He refers it as a “quiet tsunami” — a disease so silent that individuals heading toward a personal health crisis often don’t even realize it’s happening until it’s too late.
Five years ago, Nenita from Unbound’s Quezon program in the Philippines was almost one of those worst-case scenarios.
Nenita suffered from dizziness, and an unbearable pain in her stomach would sometimes cause her to faint. One of these spells that was accompanied by extreme vomiting landed her in the hospital for a week in 2020.
It was then that she learned her ailments were a result of high blood sugar and that she was diabetic.
At 79, Nenita is no longer able to work and lives with her niece’s family. Even though Nenita has been a part of Unbound’s elder sponsorship program for six years, she still couldn’t afford to properly manage her illness with the required consistent medication and care.
“In my community, we all know what diabetes is but because of poverty, some of the elderly here don’t [attend to it],” Nenita said. “They keep going even if they already know something is wrong with their body.”
Nenita’s best option for diabetes care was to monitor her diet, but she often failed at that. When she became a part of the noncommunicable diseases pilot, her health quickly began to improve.
Every three months, Nenita is transported with other sponsored elders for health checks at one of two dedicated clinics for the pilot. Not only has she learned how to proportion her meal sizes, but she’s stopped consuming products with high sugar content. She receives six-weeks’ worth of four different medications that she takes daily to help manage her high blood sugar and blood pressure, and the medications are already apportioned into daily pill boxes.
Her blood pressure, which often measured between 180-210 before, now rarely climbs beyond 130, and her dizzy spells and stomach pains have almost ceased.
“I feel like I am given the highest attention to treat my diabetes,” said Nenita about her experience in the pilot. “I am in good hands when they are talking to me.”

Unbound sponsored elder Nenita hand washes her laundry outside her home in the Philippines. Nenita has Type 2 diabetes and suffered from dizziness and extreme vomiting before joining the noncommunicable diseases pilot program in 2023.
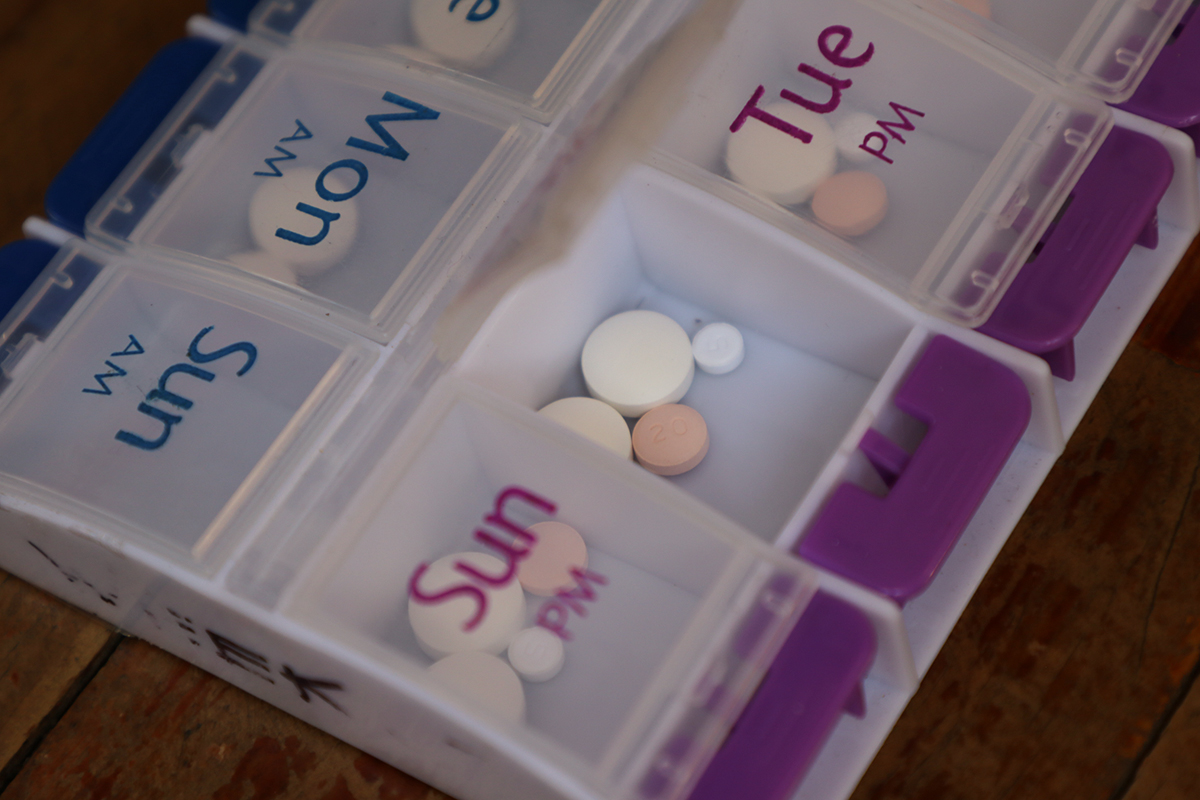
As part of the pilot, Nenita receives six-weeks’ worth of medication pre-organized into pill boxes to help her manage her diabetes. The pill boxes have been instrumental in helping the 79-year-old stay on track with taking her daily medications.

A year into the pilot program, Nenita’s blood pressure has stabilized, and she rarely experiences dizziness anymore.
A low-cost model of patient-centered care for elders with diabetes in developing countries
The CCI model of care has several components that make it effective for individuals living in poverty in developing countries.
The first component involves training a local health care team in the specific model of care. Unbound’s Quezon program staff hired one physician and five additional health care professionals who provide services to the patient participants from two sites in Quezon and Antipolo designated as clinics for the pilot.
CCI provides technical expertise and training to the local care team, visiting the pilot on a regular basis and monitoring progress through a data system, while Unbound overall provides funding for the pilot, oversight and, eventually, sponsors.
Other components to the model include sourcing generic medications to buy in bulk, educating and training patients on how to self-manage their disease, and organizing patients into small groups for peer support and accountability, among others.
“Another piece of our model is that we put the patient at the center of the care as the main driver of their health, with the realization that people’s health isn’t decided by the clinic, but by the decisions they make at home every day,” Dethlefs said.

In February 2024, members of CCI and Unbound paid a home visit to sponsored elder and pilot program participant Monica to evaluate her progress. Pictured left to right are Dethlefs, Unbound Antipolo project social worker Pilar Magnaye, Unbound Quezon program physician Isabella Bunag, Monica and her daughter Evangeline.
PILOT OUTCOMES: The elder who embraced self-management care
In the Philippines, diabetes is the fourth leading cause of mortality, where more than 4.3 million adults live with the disease, according to the International Diabetes Federation.
These statistics are one of the reasons Unbound chose its Quezon program in the Philippines as the focus for the noncommunicable diseases pilot, Pearson said. Diets in the Philippines are often high in salt and processed foods, making for a hypertensive population.
Following a healthy eating pattern is an important part of managing diabetes, which is why educating patients falls under the patient-centered care model.
Sponsored elder Geronimo took this training to heart when he joined the pilot.
For most of his life, Geronimo was a taxi driver. On the road constantly, the 66-year-old mainly consumed candy and rice when he was hungry.
When he started experiencing dizziness and numbness in his hands and feet at times, he chalked it up to aging. It was only when he was being screened for the pilot that he discovered he had Type 2 diabetes.
“Diabetes for me is a silent killer,” Geronimo said. “I keep on thinking, ‘How did I get it, and where does it come from?’ Because no one in my family has a history of diabetes.”
Geronimo takes two types of medicines to control his blood sugar and cholesterol, and he gets refills from the pilot program office every three months; but the most important thing he’s taken away from the pilot program is how to self-manage his care.
He learned how to control his diet and portion his food. He and his wife, Marilyn, jog a couple times a week for exercise, and they started a rooftop garden at their home where they grow fresh vegetables.
Geronimo’s diligence at self-managing his disease has begun to pay off — his quality of life has improved. He no longer feels dizzy and the numbness in his limbs has lessened.

Unbound sponsored elder and pilot program participant Geronimo with his wife, Marilyn, pictured in front of their home in the Philippines. The couple jog together a couple times a week now after participation in the pilot program taught Geronimo the importance of exercise in managing his diabetes.

Geronimo and Marilyn’s home in the Philippines doubles as their business, a convenience store where they also sell freshly baked bread. They made the top of their home into a rooftop garden to grow fresh vegetables they both eat.

In his rooftop garden, 66-year-old Geronimo pauses for a photo with his pet chicken.

Geronimo climbs the ladder to his rooftop garden several times a day to tend his plants, including the activity as part of his daily exercise. He grows tomatoes, eggplants, gourds, pineapple and aloe vera.
Impact that could change the face of diabetes care in developing countries
Since the noncommunicable diseases pilot between CCI and Unbound began more than a year ago, the impact has exceeded expectations, surpassing the outcomes of other partners that CCI has worked with on similar pilot programs.
To measure success, CCI breaks down data into three areas: productivity (number of patients seen), process measures (number of patients up to date on lab tests, A1C tests, checkups, etc.) and outcomes measures (patients’ ability to control their diabetes).
According to Dethlefs, for process measures in health care, it’s understood in the medical community to never shoot for 100% of anything, but to instead aim for a more realistic goal of 70-80%.
But for Unbound, the process measures for patients in the pilot is at 100% of the population, a kind of success that Dethlefs said is unheard of.
“They’re getting the job done and getting the patients the services they need,” Dethlefs said. “It really is that marriage of Unbound as the social support organization along with a health care team trained on this model of care that’s impacting what we’re accomplishing together.”

Dethlefs shares a laugh with Pilar Magnaye, a social worker with Unbound’s Antipolo program, and Isabella Bunag, a physician and member of the pilot health care team with Unbound’s Quezon program, during a home visit to a pilot participant in February 2024. The high-functioning nature of the local Unbound teams has been credited as one reason for the success of the pilot.
Pearson said staff in Unbound’s Quezon program and the pilot health care professionals are a high-functioning team, but their diligence and organization are not the only reasons for the pilot’s success thus far.
In Pearson’s experience, diabetics that live in poverty in developing countries often don’t have access to the basic tests and medicines that people in the U.S. do.
For example, families often lack access to devices that test their A1C levels. The A1C lab test shows the average level of blood sugar (glucose) over the previous three months, which helps an individual understand how well they are controlling their blood sugar so they can avoid complications from diabetes.
Pearson said the health care team’s goal was for 80% of patients in the pilot to have their A1C levels managed in phase one. For most patients, it’s the first time many have had regular access to the basic drugs that help manage their A1C levels, and it’s paying off. So far, 90% of patients have their A1C levels managed.
“CCI has really made this a rich partnership for us because they already understood us so well, and the team in Quezon has gone above and beyond,” Pearson said.
“It really pays off when you see people whose lives were pretty rapidly declining [from diabetes] be able to stabilize and recover with relatively little intervention; it’s not too complicated or costly, it’s just having focused attention to their needs.”
An area of challenge for the pilot study has been in lowering patients’ high blood pressure, which is key to preventing serious health complications like heart attacks and strokes in individuals with diabetes. Dethlefs believes this is due to the saltiness in diets in the Philippines. Patients have seen steady, albeit slow, improvements in their blood pressure levels throughout the first year of the pilot.
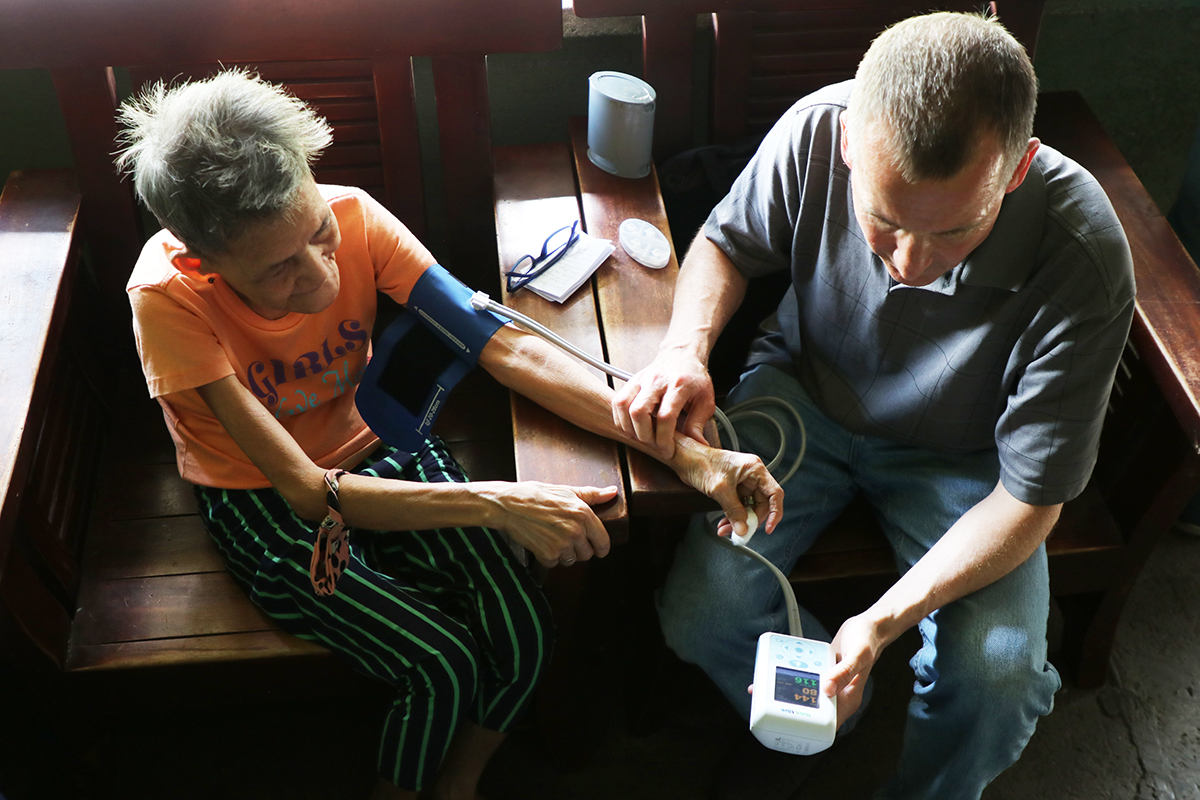
Dethlefs takes the blood pressure of sponsored elder and pilot participant Monica at her home in the Philippines.

Sponsored elder Nenita shares a look at the pre-organized pill boxes she receives as part of the pilot program. Pre-organizing medication into pill boxes for diabetes patients is one of the new strategies the Unbound and CCI teams deployed for the pilot in the Philippines, and it’s successfully helping patients better self-manage the disease.

A TRUE METRIX® monitoring device is used to measure the glucose levels of an elder patient in the pilot program and is the kind of device individuals with diabetes who live in poverty generally lack access to.
Phase two seeks to improve health outcomes for U.S. sponsors with diabetes
Phase two of CCI and Unbound’s noncommunicable diseases pilot will soon get underway. But the focus this time will not only be on sponsored individuals with diabetes in developing countries.
Phase two of the pilot shifts to a focus on U.S. individuals with diabetes who might have an interest in sponsoring an elder in the Philippines who also suffers from the disease.
Relationships have always been at the heart of Unbound, and phase two of the noncommunicable diseases pilot will add a new spin on that concept — creating positive health outcomes via peer support for sponsors and sponsored friends with diabetes.
“Research indicates that social connections combined with altruism can improve the management and health outcomes of people with diabetes,” Pearson said. “Sponsorship is both of those things — it’s social connection for the sponsor, and it’s the sponsor showing generosity.”
For as little as $40 a month — the cost of one sponsorship through Unbound — 100-150 people in the U.S. who have been diagnosed with diabetes will each sponsor one new diabetes patient in the Philippines.
While sponsor and sponsored friend form a relationship via correspondence and act as mentors to each other through their struggles with the disease, the health outcomes of both will be evaluated over a 12-month period by a research team from the University of North Carolina at Chapel Hill.
While phase two of the pilot studies a unique model of peer support for individuals who suffer with diabetes, both Dethlefs and Pearson have faith in its potential impact. The CCI team has briefly tested and seen success from a version of this model already in the Dominican Republic.
Dethlefs said diabetes is a challenging illness for anyone, no matter what country they live in or their circumstances.
“One of the reasons I love this work is because I think one of the most important things any of us can do is to facilitate the development of authentic community,” Dethlefs said. “Diabetes is such an impactful disease to have that it creates this foundation of commonality between those who have it.
“We’ve really grown to see this peer support model as an opportunity for community.”
Are you living with diabetes in the U.S. and think you might have an interest in the noncommunicable diseases pilot? Learn more about phase two of the pilot.

Sponsored elder Nenita’s quality of life has improved since joining the noncommunicable diseases pilot in 2023, and she cherishes the time she gets to spend with her grandchildren. Pictured is Nenita with her grandchildren, Lyka (left) and Aisha.
Regional Reporter Teejay Cabrera contributed information and photos for this story.